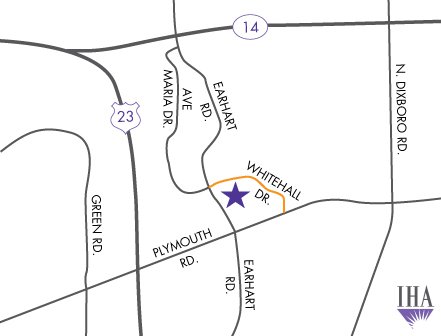
If you have an appointment at IHA Domino’s Farms Medical Center, or need to visit the urgent care this Saturday, October 15; please use Whitehall Dr. The annual Defeat Depression Dash will be running their 5k on Earhart Rd., which will be closed to traffic prior to 9:00 am, which is when their race starts. Learn more: http://www.nndc.org/get-involved/annual-defeat-depression-dash/
IHA Pediatric Medicine
Are you looking for care for your child? We have over 80 providers in 14 locations.
Locations
IHA Canton Pediatrics – Heritage Park
IHA Pediatric Healthcare – Arbor Park
IHA Pediatric Healthcare – Canton
IHA Primary Pediatrics – Domino’s Farms
The following locations have at least one internal medicine & pediatric physician, which means the physician can see both pediatric and adult patients.
IHA Family & Internal Medicine – Howell
IHA Family & Internal Medicine – WestArbor
Flu Vaccine Updates
We strongly encourage you and your family be vaccinated! For ease of convenience, we’re offering all flu shots to be scheduled online, or by calling your office directly. When scheduling them online, please schedule one person per appointment time. If you have questions or concerns, please contact your physician’s office.
Peripheral artery disease and IHA’s outpatient endovascular center
Peripheral artery disease (PAD) is a blood disease of the legs, where plaque builds up in the arteries.
Plaque is made up of fat, cholesterol, calcium and other substances in the blood. When you develop PAD your extremities, usually your legs, don’t receive enough blood flow, which causes symptoms such as leg pain or calf cramping when walking. You have a higher chance of contracting PAD if you have diabetes and/or smoke.
Most cases of PAD are treatable, although in very serious cases, PAD can lead to leg amputation. At IHA Vascular & Endovascular Specialists, we have an outpatient center equipped to perform the most up-to-date procedures for PAD, if it’s necessary. We try non-surgical options first, such as a medication and lifestyle changes, and work our way toward surgery if it’s needed.
In our outpatient endovascular center, we can perform many minimally-invasive procedures, which will allow the patient to avoid the hospital. We also strive to perform minimally-invasive procedures, which allows the patient less downtime and a faster recovery.
If you have leg pain when you walk or climb stairs, talk to your doctor. Some older adults associate leg pain with the aging process; however the cause of pain could be PAD.
This article was originally published on April 7, 2016, and was updated on September 19, 2016.
Welcome Kavita Warrier, MD, FAAP

Please join us in welcoming Kavita Warrier, MD, FAAP, to IHA Canton Pediatrics – Heritage Park. Dr. Warrier is a board-certified pediatrician. She has clinical interests in children with complex, chronic health conditions, premature infants and cerebral palsy. To learn more about Dr. Warrier, or to schedule an appointment, click here.
Join us for IHA WestArbor Open House!

Join us on Sunday, September 25 from 2:00 – 4:00 pm for an open house at Ann Arbor’s newest medical center, IHA WestArbor Medical Center.
- Meet providers and staff
- Tour the facility
- Balloon artist
- Raffles and giveaways
- Live broadcast with Ann Arbor’s 107one
Join our IHA Pokémaster and continue your hunt to catch ’em all!

Making Halloween safe and inclusive for kids with allergies

When a child has food allergies, Halloween can be a scary time. The small candy wrappers often do not contain lists of ingredient, making it nearly impossible to make sure your little one is eating a treat that’s safe for them. When your child has an egg, milk, nut or soy allergy, how do you make sure they’re safe and can have a fun Halloween experience?
The Food Allergy Research & Education (FARE) organization started the Teal Pumpkin Project, which encourages people to place a teal painted pumpkin outside their door if they’re offering non-food treats, such as stickers or small toys, to trick-or-treaters.
It’s a small step to make sure all children can be a part of the fun on Halloween, and it allows the parent to know their children will be safe without a bag full of candy they may or may not be able to eat safely.
If you’re interested in participating, it’s very simple! Place a teal painted pumpkin outside your door to let trick-or-treaters and their parents know you have non-food items, and pass them out like you normally would. Some kids may ask for them knowing they can’t have dairy, soy or nuts. It’s best to keep the non-food treats in a separate bowl or container, so extra safety from cross-contamination. FARE has printable materials available for you to display to let others know there are non-food items available at your home.
This article was originally published on September 30, 2015, and was updated on September 7, 2016.
2nd Annual Women’s Health Symposium

SATURDAY, OCTOBER 8, 2016 | 8:00 am – 12:30 pm | Check-in starts at 8:00 am | FREE EVENT
Ann Arbor Marriott Ypsilanti at Eagle Crest | 1275 S. Huron St., Ypsilanti, MI 48197
 Featuring nationally recognized keynote speaker and time management expert Mary LoVerde, who will be teaching women a new work-life balance approach in her humorous and fast-paced presentation, I Used to Have a Handle on Life, But it Broke.
Featuring nationally recognized keynote speaker and time management expert Mary LoVerde, who will be teaching women a new work-life balance approach in her humorous and fast-paced presentation, I Used to Have a Handle on Life, But it Broke.
For fifteen years, as a busy mother with a demanding career, Mary LoVerde tried the ‘superperson’ route and failed. Struggling to keep up, she turned to time management, delegating and simplifying. Yet, she continued to feel overwhelmed. One day, while furiously working away at her computer and shouting at the kids, she realized a startling fact. In her zeal to get everything done, she had become disconnected — from her family, from her work and from the person she was and wanted to be. LoVerde adopted a new life motto: When you can’t keep up, CONNECT.

Breakout session ONE
Parenting 101: Baby Basics and Love and Logic OR Behavioral Health: Coping with Life Transitions
Breakout session TWO
What is Normal? Understanding Routine Gynecological Findings OR Pelvic Floor Treatment Options
Breakout session THREE
Prenatal Counseling, Fertility and Genetic Education OR Breast Health
Featuring keynote speaker, breakout sessions, vendor tables, refreshments & more!


Vendor Sponsors:
ClinSite
HealthPlus Pharmacy
Inspirit Salon & Spa
MOVE
Myint Family Chiropractic
Natera
Parros College Planning LLC
Progenity
Saint Joseph Mercy Breast Imaging
Sapphire Therapeutic Spa
Sequenom Laboratories
St. Joseph Mercy Health System, Ann Arbor, Breast Health Risk Reduction programs
Welcome Tara M. Breslin, MD, FACS

Please join us in welcoming Tara M. Breslin, MD, FACS, to IHA Breast Surgery – Ann Arbor and IHA Breast Surgery – Brighton. Dr. Breslin is a board-certified surgeon who specializes in breast surgical oncology. She has been in practice for over 16 years, and her clinical expertise revolves around the diagnosis and treatment of benign and malignant breast disease and evaluation of women at increased risk for breast cancer. To learn more about Dr. Breslin, click here.
Welcome Shahbaz Nisar, MD

Please join us in welcoming Shahbaz Nisar, MD, to IHA Family Medicine – Arbor Park. Dr. Nisar has clinical interests in preventive care and special procedures including laceration repair and toenail removal. He is welcoming new patients and < a href="https://iha.inquicker.com/provider/shabaz-nisar">scheduling appointments online.


